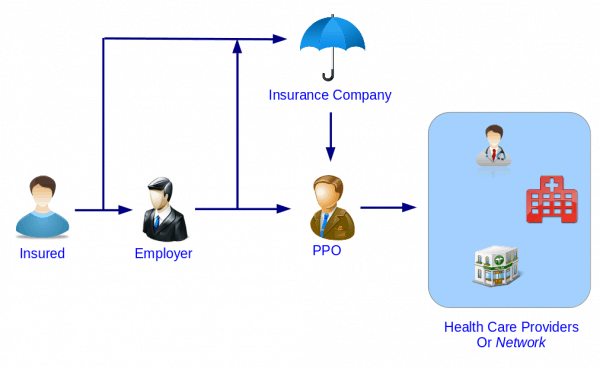
With a PPO, though, you may have more than one deductible to meet. 
Once you’ve paid a total of $1,200 for medical costs, your insurer will cover future costs for the rest of the year, as stated in your policy documents. The amount you paid at that visit is then credited toward your deductible. After seeing you, your doctor will bill the insurance company. By contrast, HMOs and some other plans make your PCP the point person for coordinating and managing your care.Ī deductible is the amount of money you have to spend out of pocket for covered services before your insurer will pay for anything.įor example: Say your deductible is $1,200 a year. Responsibility for coordinating care: Choosing doctors and specialists directly means that you have the job of coordinating your care. If you frequently see out-of-network providers, filling out and submitting documentation could turn out to be time-consuming and frustrating. Potentially more paperwork: Going outside your PPO network may require you to submit a claim form to your insurer. For example, you may pay 20% in coinsurance for an in-network doctor and 40% for an out-of-network one. You’ll typically pay a larger coinsurance percentage for seeing a doctor outside your network. Other costs to consider: While PPO members can see any doctor or specialist, the cost-sharing rules do vary. (Among workers whose plans have a general annual deductible, the averages for HMOs and PPOs are similar: $1,271 for HMOs, versus $1,245 for PPOs.) More likely to have an annual deductible: KFF research also found that 43% of workers in HMOs don’t have deductibles, compared to only 15% of those in PPOs. By comparison, HMO premiums were $1,204 for individuals and $5,254 for families. 
The Kaiser Family Foundation (KFF) reported that, in 2021, annual PPO plan premiums were $1,389 for individual workers and $6,428 for families paid. The price of flexibility: PPO premiums tend to be higher than those for other plan types. By contrast, HMOs typically limit you to a network in your local area. You still have coverage when you’re traveling, or if you need to see doctors and specialists out of state. Travels with you: PPO coverage protects you when you’re away from home, because you aren't limited to your network of healthcare providers. These details vary, depending on your plan. May offer more services: Some PPOs offer a wider range of services to participants, going beyond traditional checkups and preventative care to chiropractor and acupuncture services. This means there’s no doctor managing your care overall, so you don’t have to persuade anyone to give you a referral to other providers. No referrals needed: PCPs are optional in PPOs. Also, PPOs pay partial costs for out-of-network care, which frees you up to choose from a wider selection of doctors and specialists. More flexibility: Unlike with HMOs, PPOs do not require you to select a primary care provider (PCP). Here are the pros and cons of this type of plan. Nearly half of all workers are enrolled in one. PPOs are the most popular type of health insurance coverage, ahead of both health maintenance organizations (HMOs) and exclusive provider organizations (EPOs). If you choose coverage through Medicare Advantage (Medicare Part C), you can pick a PPO plan run by a private insurer. People on Medicare also have access to PPOs. Also, depending on your plan, an in-network provider visit may not require copays or other out-of-pocket costs. The “preferred” part means that participants typically pay lower fees to providers within the network. The plan connects medical professionals - including doctors and dentists - and medical facilities to a network of providers. It’s a type of health insurance plan available to individuals and families. “PPO” stands for preferred provider organization.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
